Health Effects and Recovery Timelines After Quitting Smoking: Complete 2026 Guide
You already know smoking causes lung cancer. What most people don’t realize is exactly how much that risk drops once you stop — and how quickly your body starts recovering in ways that actually show up on medical tests. The health effects and recovery timelines after quitting smoking are more dramatic than most smokers expect, beginning within minutes and compounding for years. Whether you stubbed out your last cigarette this morning or you’re still working up the courage to quit, the data on what happens next is genuinely striking.
Within 20 minutes of your final cigarette, measurable changes begin. Within 10 years, your lung cancer risk is cut roughly in half compared to someone who keeps smoking. This guide walks through every stage — the biology, the numbers, the uncomfortable withdrawal phase, and the long-term payoff — so you know exactly what to expect and when.
Table of Contents
- What Happens When You Quit Smoking: Hour-by-Hour
- Quit Smoking Benefits Timeline: Days to Decades
- Nicotine Withdrawal Symptoms: What to Expect
- Nicotine Withdrawal Timeline: Week by Week
- Lung Cancer Risk Reduction After Quitting
- Comparing Quitting Methods: NRT, Medication, Behavioral Support
- Practical Quit Plan: Your First 30 Days
- Frequently Asked Questions
What Happens When You Quit Smoking: Hour-by-Hour
The body is remarkably good at repair — it just needs you to stop creating new damage. Here’s where the science gets specific about what happens when you quit smoking in the earliest hours.
Definition: Smoking Cessation
Smoking cessation refers to the complete discontinuation of tobacco product use, including cigarettes, cigars, and pipes. From a clinical standpoint, it’s defined as sustained abstinence — typically 7 days or more — confirmed by self-report or biochemical verification such as exhaled carbon monoxide testing.
20 minutes: Your heart rate and blood pressure begin to drop toward normal ranges. Peripheral circulation improves — hands and feet start warming up. This isn’t anecdotal; it’s measurable with a blood pressure cuff.
2 hours: Nicotine levels in the bloodstream drop enough to trigger the first withdrawal signals in many smokers. Some people notice mild irritability or restlessness. This is actually evidence the process is working.
8–12 hours: Carbon monoxide — the same gas that makes car exhaust dangerous — clears from your blood. Oxygen levels normalize. This is one of the fastest and most physiologically significant changes that occurs after quitting.
24 hours: Your risk of having a heart attack begins to decline. The American Cancer Society notes that within just one day, the damaged nerve endings in the nose and mouth start to regenerate, which is why many ex-smokers report food tasting different within days of quitting.
48 hours: Nerve endings continue regenerating. Smell and taste perception noticeably improve for most people. No nicotine remains detectable in the blood (though cotinine, a nicotine metabolite, may persist in urine for several more days).
72 hours: Bronchial tubes relax and begin to widen. Breathing feels physically easier for many people — sometimes the first concrete sign that something real is changing. This is also, for many smokers, the hardest withdrawal day.
Quit Smoking Benefits Timeline: Days to Decades
The quit smoking benefits timeline is one of the most compelling arguments for cessation — not because the short-term gains are dramatic, but because the cumulative effect over years is genuinely extraordinary.
| Time After Quitting | Health Benefit | Clinical Significance |
|---|---|---|
| 20 minutes | Heart rate and blood pressure drop | Reduced acute cardiac workload |
| 12 hours | Blood carbon monoxide normalizes | Full oxygen-carrying capacity restored |
| 2–12 weeks | Circulation improves; lung function increases up to 30% | Reduced shortness of breath during exercise |
| 1–9 months | Cilia regrow in airways; mucus clearance improves | Reduced respiratory infections, less chronic cough |
| 1 year | Coronary heart disease risk cut by ~50% | Major cardiovascular risk reduction |
| 5 years | Stroke risk equal to a non-smoker | Cerebrovascular risk fully normalized |
| 10 years | Lung cancer risk ~50% of a current smoker’s | Significant oncological risk reduction |
| 15 years | Coronary heart disease risk equal to non-smoker | Cardiovascular risk fully normalized |
Sources: CDC — Benefits of Quitting Smoking; National Cancer Institute Cessation Fact Sheet
Here’s where it gets interesting: the 2–12 week window often surprises people most. A 30% improvement in lung function sounds abstract until you climb a flight of stairs without wheezing. These are functional changes, not just statistical ones.
The 1–9 month period involves a process that most people don’t know about: cilia regrowth. Cilia are the tiny hair-like structures that sweep mucus, debris, and pathogens out of your airways. Smoking paralyzes and destroys them. As they regenerate post-cessation, many ex-smokers experience a temporary increase in coughing — which is actually a good sign. The system is coming back online.
For anyone with a family history of heart disease or stroke, the 5-year milestone represents one of the strongest arguments for quitting. By year five, your stroke risk reaches the same level as someone who never smoked. The body’s capacity to reverse vascular damage — given enough time — is remarkable.
Nicotine Withdrawal Symptoms: What to Expect
Nicotine withdrawal is real, measurable, and — critically — temporary. Understanding exactly what it involves takes away a significant part of its power.
Nicotine works by mimicking acetylcholine receptors in the brain and triggering dopamine release. After years of regular exposure, the brain upregulates these receptors, essentially becoming dependent on nicotine to maintain normal dopamine levels. When nicotine is removed, the system has to recalibrate — and that recalibration process produces the symptoms most people associate with “needing” a cigarette.
Definition: Nicotine Dependence
Nicotine dependence is a substance use disorder recognized in DSM-5 (Tobacco Use Disorder), characterized by compulsive use despite harm, tolerance, withdrawal symptoms on cessation, and failed attempts to stop. It involves both physical dependence (neurochemical adaptation) and psychological dependence (habitual cue-response patterns).
The physical nicotine withdrawal symptoms typically include:
- Intense cravings — usually peaking at 3–5 minutes per craving episode, despite feeling much longer
- Irritability and frustration — driven by dopamine dysregulation, not personality
- Anxiety and restlessness — particularly pronounced in smokers who used cigarettes for stress regulation
- Difficulty concentrating — cognitive performance genuinely dips during acute withdrawal; this is temporary
- Increased appetite and weight changes — nicotine suppresses appetite; without it, hunger signals normalize
- Sleep disturbances — insomnia, vivid dreams, or excessive sleepiness are all documented during the first week
- Headaches — often from vasodilation as blood vessels relax
- Constipation or gastrointestinal changes — nicotine stimulates the gut; its absence can temporarily slow digestion
The symptom list looks intimidating. But a systematic review published in PMC examining decades of epidemiological data found that the peak of physical withdrawal — the hardest days — typically lasts 72 hours or less for most symptoms. The psychological component runs longer, but it’s manageable with the right support.
For people managing withdrawal, exploring effective quitting strategies and managing withdrawal symptoms in tandem with understanding the biology makes a significant difference in outcomes. Knowing the mechanism behind a symptom reduces the panic it creates.
Nicotine Withdrawal Timeline: Week by Week
The nicotine withdrawal timeline varies by individual — how heavily you smoked, how long you smoked, your baseline anxiety levels, and whether you’re using cessation aids all affect the curve. That said, there’s a general pattern that holds across most clinical data.
Hours 0–24: The Opening Phase
Cravings begin within 30–60 minutes for heavy smokers. Irritability and mild anxiety appear by hour 2–3. Physical symptoms — headache, slight nausea, difficulty concentrating — may begin in the late morning or afternoon of day one. Most people report day one as moderate; the real test comes next.
Days 2–3: Peak Withdrawal
This is statistically the hardest period. Dopamine deficit is at its most pronounced. Cravings are most frequent and intense. Sleep may be disrupted. Appetite increases. Some people experience what feels like a low-grade flu — fatigue, mild dizziness, a foggy quality to thinking.
This is also the window with the highest relapse risk — and it’s worth understanding why. The discomfort peaks before the benefits become noticeable, which creates a frustrating gap. The body is working hard; the reward isn’t visible yet.
Days 4–7: Stabilization Begins
Physical symptoms start easing for most people. Headaches become less frequent. Sleep begins normalizing. Cravings become shorter and more manageable. By day 5 or 6, many people report windows of several hours where they aren’t thinking about cigarettes at all — often for the first time.
Weeks 2–4: The Psychological Phase
Physical dependence is largely resolved by the end of week one for most people. What remains is behavioral conditioning — the habit loops, the contextual triggers, the “I always smoke after coffee” associations. This phase is subtler and often catches people off guard precisely because they feel physically fine.
Stress events — a bad day at work, an argument, a long commute — are high-risk moments in weeks two through four. The brain still has deeply ingrained pathways associating those situations with lighting up.
Months 2–6: Long-Term Craving Management
Cravings at this stage are typically infrequent and brief — triggered by specific situations rather than constant neurochemical need. The brain is forming new baseline dopamine patterns without nicotine. Weight changes may continue stabilizing. Most people report that by month three, they feel functionally normal without cigarettes.
| Timeline | Primary Withdrawal Features | What Helps Most |
|---|---|---|
| Hours 0–24 | First cravings, mild irritability | NRT, hydration, distraction |
| Days 2–3 | Peak cravings, sleep disruption, fatigue | NRT, medication (varenicline/bupropion), support |
| Days 4–7 | Symptoms easing, appetite increase | Exercise, healthy snacking, routine |
| Weeks 2–4 | Behavioral triggers, mood variability | Behavioral therapy, trigger identification |
| Months 2–6 | Occasional situational cravings | Mindfulness, continued social support |
Lung Cancer Risk Reduction After Quitting
Lung cancer is the leading cause of cancer death in the United States — and smoking accounts for approximately 80–90% of cases. The risk doesn’t disappear overnight after quitting, but it does drop meaningfully, and continuously, with time.
A 2020 systematic review published in PMC examining epidemiological evidence from high-income countries confirmed that former smokers show substantially lower lung cancer rates than current smokers across all age and pack-year categories. The magnitude of risk reduction depends on several factors:
- Age at quitting: Quitting before age 40 reduces the excess risk of dying from smoking-related causes by approximately 90%. Quitting at any age provides benefit.
- Pack-year history: Someone who smoked a pack a day for 30 years carries higher residual risk than someone who smoked half a pack for 10 years — even with equal years of cessation.
- Years since quitting: Risk reduction is continuous and cumulative; it doesn’t plateau early.
What’s the mechanism? Cigarette smoke contains over 70 known carcinogens, including polycyclic aromatic hydrocarbons, nitrosamines, and benzene. These compounds cause DNA mutations in lung cells. The longer smoke exposure continues, the more mutations accumulate. After cessation, the mutation rate stops increasing, and the body’s DNA repair mechanisms begin — slowly — correcting damage. Cells with mutations can still develop into cancer, which is why residual risk doesn’t drop to zero immediately, but the trajectory is consistently downward.
One piece of data that tends to motivate current smokers: quitting at age 50 still cuts the risk of lung cancer death by roughly 50% compared to continued smoking. Quitting at 60 still provides substantial benefit. There’s no point in a smoker’s career where quitting stops being worth it.
Comparing Quitting Methods: NRT, Medication, Behavioral Support
Cold turkey gets romanticized, but the data tells a different story. Most people who quit successfully do so with some form of support — and combining approaches consistently outperforms any single method.
Nicotine Replacement Therapy (NRT)
NRT delivers controlled doses of nicotine without the thousands of toxic combustion compounds in cigarette smoke. Forms include patches, gum, lozenges, inhalers, and nasal spray. NRT roughly doubles quit rates compared to placebo. Combination NRT — patch plus a faster-acting form like gum or lozenge — is more effective than a single NRT type alone.
One thing people get wrong: NRT patches deliver nicotine at a much slower rate than cigarettes. The “hit” is absent. That’s actually the point — it maintains just enough nicotine to blunt withdrawal while the brain begins recalibrating.
Prescription Medications
Varenicline (Chantix/Champix): A partial nicotinic receptor agonist that both reduces withdrawal symptoms and blunts the reward of smoking. The highest-efficacy single pharmacotherapy available, with trial data showing continuous abstinence rates roughly three times higher than placebo. Carries warnings about mood changes in some patients — worth discussing with a physician.
Bupropion (Wellbutrin/Zyban): Originally an antidepressant, bupropion was found to significantly reduce cravings and improve quit rates. Particularly useful for smokers with comorbid depression. Roughly doubles quit rates versus placebo.
Behavioral and Digital Support
Behavioral counseling — whether individual, group, or digital — is independently effective and adds benefit when combined with pharmacotherapy. The American Cancer Society’s guide to quitting tobacco provides a strong framework, including the 5 A’s model used in clinical settings.
Digital tools have strong evidence behind them — particularly text message programs and app-based interventions. The NCI’s Smokefree.gov tools (including QuitGuide, quitSTART, and SmokefreeTXT) are free, evidence-based, and accessible without a prescription.
| Method | Evidence Level | Best For | Notes |
|---|---|---|---|
| Cold turkey | Moderate (lower success rate) | Low-dependence smokers | ~5% unaided success at 12 months |
| NRT (single) | Strong | Moderate dependence | Doubles quit rates vs. placebo |
| Combination NRT | Strong | Heavy smokers | Patch + short-acting form |
| Varenicline | Strongest | Heavy/long-term smokers | Prescription required; discuss with doctor |
| Bupropion | Strong | Smokers with depression | Prescription required |
| Behavioral counseling | Strong (additive) | All smokers | Best combined with pharmacotherapy |
| Digital support apps | Growing evidence base | All smokers; tech-comfortable users | 24/7 access; real-time tracking |
For detailed tactics on building a quit plan that sticks, the resource at quit smoking strategies and overcoming triggers covers the behavioral science behind successful cessation in practical detail.
The Mayo Clinic’s guide to quitting smoking also includes a frank discussion of why quitting is so physiologically difficult — useful for both smokers and the people supporting them.
Practical Quit Plan: Your First 30 Days
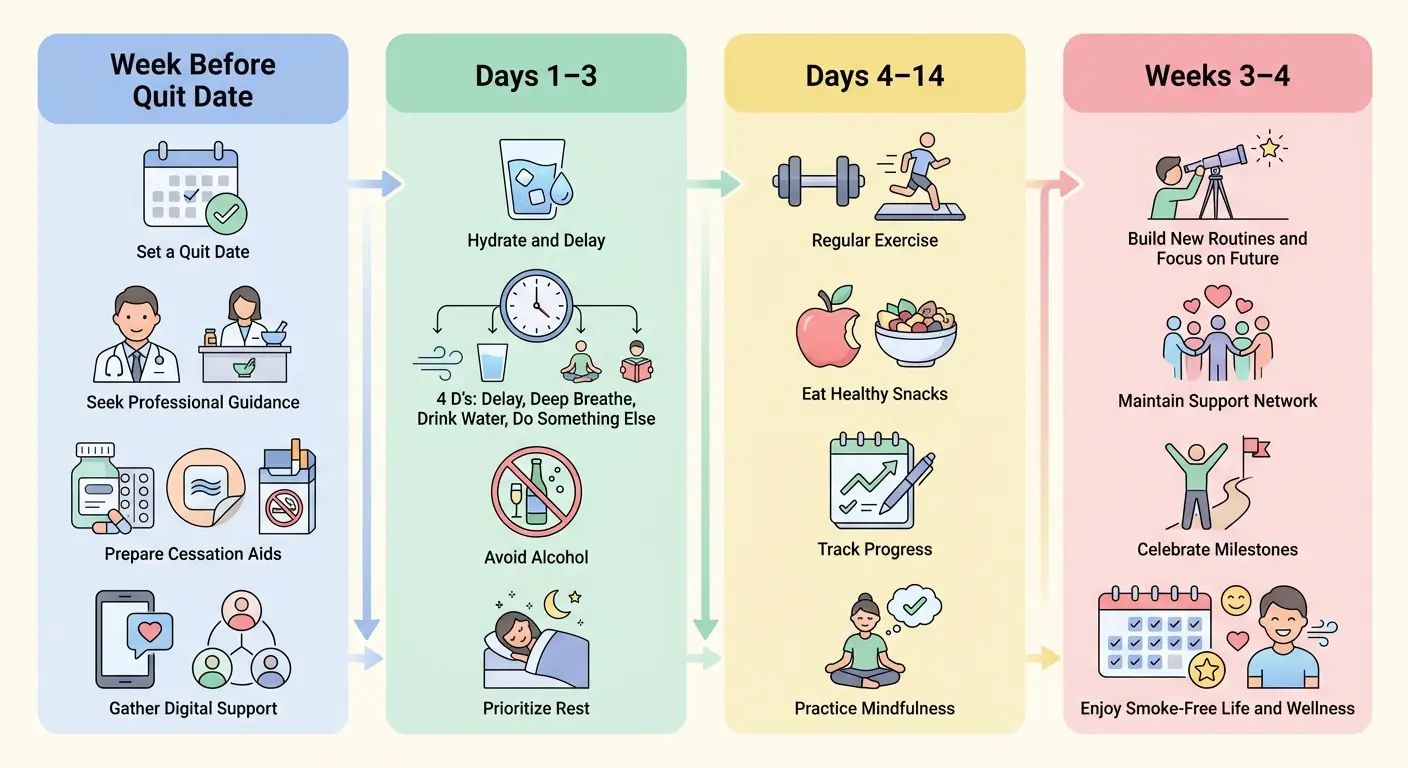
Most quit attempts fail in the first two weeks — not because of willpower deficits, but because of inadequate preparation. Here’s a structured approach to the first 30 days based on the evidence.
Week Before Your Quit Date
- Set a specific quit date — within 2 weeks of today. Too far away and motivation wanes; too soon and preparation suffers.
- Identify your triggers — coffee, driving, stress, after meals, social situations. Write them down. Triggers you’ve named are triggers you can prepare for.
- Choose your support method — NRT, medication, digital tool, counseling, or a combination. Don’t wing it.
- Remove cigarettes, lighters, ashtrays — from home, car, and workplace the night before your quit date. Friction matters.
- Tell at least one person — social accountability is independently associated with higher quit rates. A single supportive person changes the math.
Days 1–3: Peak Withdrawal Management
- Start NRT or medication on quit day — not the day before, not “when it gets bad.”
- Use the 4 D’s for cravings: Delay (wait 5 minutes), Deep breathe, Drink water, Do something else.
- Avoid alcohol — alcohol is the single strongest behavioral trigger for relapse in early cessation.
- Plan your first two days carefully — this is not the time to attend a party where people smoke.
- Track your progress — even a simple note on your phone. Seeing “72 hours smoke-free” is motivating.
Days 4–14: Building the New Pattern
- Replace the ritual, not just the nicotine — if you smoked outside after dinner, take a walk instead. The behavior slot matters.
- Manage weight proactively — healthy snacks, regular meals, increased water intake. Don’t fight both withdrawal and hunger.
- Start or increase exercise — even 20 minutes of walking reduces craving intensity and improves mood. This isn’t motivational filler; it’s supported by clinical data.
- Expect the cough — many people experience increased coughing around days 5–10 as cilia regrow. It means your lungs are working.
Weeks 3–4: Navigating Psychological Cravings
- Identify high-risk situations in advance — upcoming stressors, social events, travel. Plan your response before you’re in the moment.
- Journal mood and energy — patterns often reveal specific triggers that were invisible before.
- Celebrate the 2-week mark — genuinely. Lung function has already begun improving. Circulation has measurably changed. These are real physiological achievements.
- Revisit your “why” — write it down before day one and read it on day 21. The reasons don’t change; your access to them does.
- Quit date chosen and committed
- Triggers identified and documented
- Support method selected (NRT, medication, app, counseling)
- Cigarettes removed from all environments
- At least one accountability person informed
- High-risk situations for first week mapped out
- Craving strategy ready (4 D’s, distraction plan)
- Progress tracking method in place
- Doctor or pharmacist consulted about cessation aids
- Lung cancer screening eligibility checked (if applicable)
Frequently Asked Questions
How long does nicotine withdrawal last?
Physical nicotine withdrawal symptoms — including intense cravings, irritability, and difficulty concentrating — typically peak at 48–72 hours and largely resolve within 1–2 weeks. Psychological cravings and behavioral triggers can persist for weeks to months, but their intensity decreases significantly after the first month. Most people report feeling functionally normal without cigarettes by month two to three.
Does lung cancer risk go back to normal after quitting smoking?
Not fully, but it drops substantially. After 10 years of abstinence, lung cancer risk is approximately 50% that of a current smoker. After 15–20 years, risk approaches — but may not fully equal — that of a lifelong non-smoker, depending on cumulative exposure (pack-years). Quitting at any age meaningfully reduces risk; earlier cessation provides greater long-term benefit.
What happens to your lungs in the first year after quitting smoking?
Within 2–12 weeks, lung function improves by up to 30% and circulation to the lungs increases. Over 1–9 months, cilia — the hair-like structures that clear mucus and debris from airways — regenerate, reducing respiratory infections and chronic cough. By the one-year mark, the airways are significantly cleaner and more functional, and the risk of COPD exacerbation drops for those with existing lung disease.
Is it normal to cough more after quitting smoking?
Yes — and it’s actually a sign of recovery, not damage. As cilia regrow in the bronchial passages (typically weeks 1–4 after quitting), they become active and begin sweeping accumulated mucus and debris out of the airways. This process temporarily increases coughing and mucus production. For most people, this resolves within 4–8 weeks and is followed by noticeably easier breathing.
What is the best method for quitting smoking?
Combination approaches outperform any single method. The strongest evidence supports varenicline (a prescription medication) as the most effective single pharmacotherapy, with quit rates roughly three times higher than placebo. Combining medication or NRT with behavioral counseling — whether in-person, via phone, or through a digital tool — consistently produces better outcomes than medication alone. “Cold turkey” works for some people, but the success rate is significantly lower.
Will I gain weight after quitting smoking?
Weight gain after quitting smoking is common but typically modest — an average of 4–10 pounds in the first year, according to research data. Nicotine
Start Your Smoke-Free Journey
iQuit gives you everything you need to quit smoking for good.